Blog
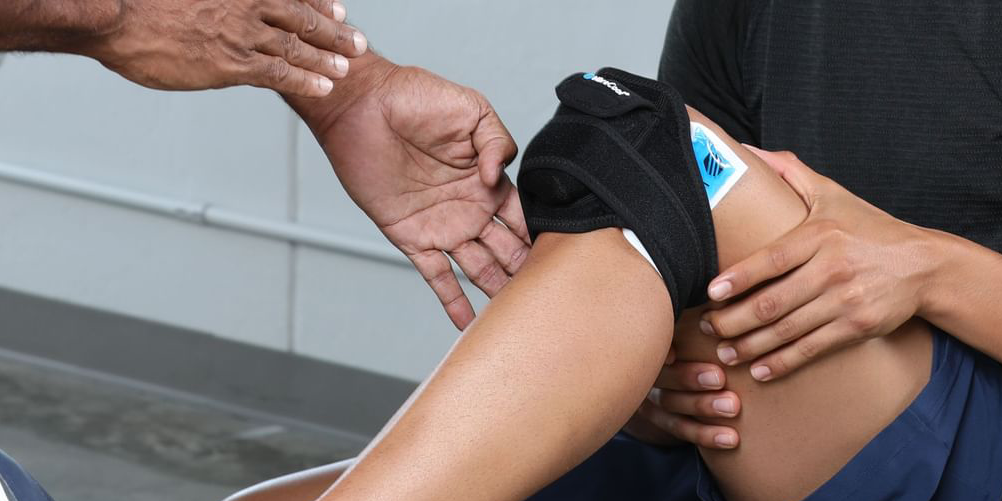
Translating New Pain Management Research For Patients – (1 of 3) A. Baxter MD
Translating New Pain Management Research
Part 1: What Is Pain?
Imagine hitting your hand with a hammer. Since the discovery of the nerve, pain has been portrayed as an impulse traveling from hand to head, with concrete implications: if you can stop the transmission in the hand, as with lidocaine, there is no pain.
If you can block pain in the spine, the brain is blissfully unaware. And most recently, if a medicine blurs the reception of pain in the brain, the problem is solved. Pain is an alarm system that can be short-circuited.
New Pain Management Studies
New functional MRI (fMRI) studies have changed the way we understand nociception (perception of noxious stimuli). Instead of an all-or-none pain bolus from the periphery in a tidy 0-10 rating, pain is a nuanced interpretation of both the stimulus and the context.
Being knocked to the ground in an attack can be a scary, painful event. When you’ve just caught a football and you’re tackled in the end zone, pain is irrelevant. When a child is awaiting their third injection, the screaming may begin with a benign swipe of an alcohol wipe.
New theories of pain have recast the nature of the sensation itself. The notion that “Pain is the brain’s opinion of how safe it is” maintains the alarm system metaphor, adding the nuance that alarms can be muted. The idea that “Pain is an emotion” elevates the brain’s role in mitigating pain, and acknowledges that it’s quite real while underscoring the factors that make emotions stronger: fatigue, hunger, fear, repetition.

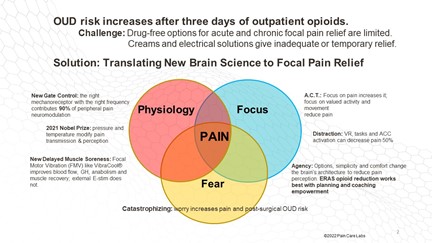
Putting these concepts together allows for clinical advances and hope for those with chronic pain. Pain Care Labs’ construct is that modern pain management addresses the physiology, fear, and focus.
Physiology Pain Management
There are four touch receptors – light touch, deep pressure, position sense, and stretching. Researchers used to think that any of these “mechanoreceptors” sensations would outrace pain to the spine to shut it out. Our “Gate Control” understanding has grown more sophisticated. When someone smashes their thumb with a hammer, light stroking doesn’t help. Vigorous shaking of the position sense nerves do the trick, and we now know the frequencies to mimic position sense Pacinian nerves.
Focus Pain Management
Previous pain research concentrated on measuring pain often, with the unfortunate side effect of drawing attention to injury or disability. Just as your hearing becomes more acute concentrating on the sound of a possible intruder, focusing on pain enhances the sensation.
Instead, new therapies like Acceptance and Commitment Therapy (ACT) focus on making movement and activity goals. By gauging success on enjoyment goals, pain is lessened more than it is when using traditional pharmaceutical protocols.
With acute pain, activating the executive function (anterior cingulate cortex) diminishes the perception of pain. Simple visual counting tasks on DistrACTION cards and active virtual reality are equally effective: the important components are rapid task resolution, visual engagement, and discrimination. The next time you get a vaccine, concentrate on any sentence and count the number of letters with a hole in them. “It’s going to be fine” has seven.
Fear Pain Management
If you’ve heard of the amygdala, it may be in the context of anger or fear. fMRI studies show that pain lights up the amygdala like a beacon. When the brain is trying to assess safety, it makes sense that putting fear on high alert would increase pain perception.
What may not be as intuitive is that control is the natural counterbalance of fear. When patients know they have a pain reliever in the next room, they can tolerate pain longer. Suffering pain becomes a choice, allowing them to decide when the annoyance outweighs the effort to obtain relief.
Chronic pain patients say over and over that they want options – what they want is some control and hope to smother fear. With chronic pain, areas of the brain involved in meaning also light up to ask questions, such as:
- “Will I always be like this?”
- “What if I can’t stand it and sneak a pain pill early, what does that mean?”
- “Is it supposed to hurt this much?”
- “Is it damaged?”
By giving patients options, letting them know when to expect maximal pain, and with therapeutics they control (hot, cold, intensity, position) the amygdala can stand down and pain is reduced.
Opioid Alternative for Managing Pain
There is only so much a pain pill can do. By teaching patient's tools, using empowering multimodal solutions, balancing expectations, and putting the focus on activity, we’re translating research into good patient care.
VibraCool offers an opioid alternative for pain management that is backed by research and used by clinicians nationwide. Explore VibraCool products that combine the pain-blocking power of vibration and ice.



